A new study by researchers at University of Illinois at Urbana-Champaign and Brookhaven National Laboratory and published on the preprint server medRxiv* in July 2020 discusses the effect of a factor called persistent contact heterogeneity on the final epidemic size of COVID-19. The researchers say that using estimates based on this measure reduces the herd immunity threshold (HIT) and suggests that the worst-affected areas, such as New York City (NYC), are almost at this threshold, meaning that they will not be sources of spread to other areas if a second wave of the current pandemic occurs.
.jpg)
Various Epidemiological Approaches
Epidemiological models have been important in studying the numbers and progression of infectious outbreaks, but incorporating the role of population heterogeneity in terms of individual susceptibility, as well as social networks into such studies, has been a challenge in many cases. Among the significant consequences of these factors is the occurrence of superspreader events that fuel the initial local outbreak, the alteration in the HIT, and the final size of the epidemic (FSE).
Several approaches have been adopted to include this factor while modeling the dynamics of an epidemic, focusing on various characteristics and parameters. For instance, one might use age-stratified groups to estimate variations in contacts and susceptibility. Another could use mathematical modeling to simulate real or artificial social networks.
The Unifying Theory
The current approach is aimed at predicting not the final state of the outbreak, as with the other two, but the whole changing scenario in relation to time. This has been applied to COVID-19, and many researchers have come to the conclusion that the HIT may be significantly lower than that arrived at by more conventional models based on homogeneity.
The researchers consider overdispersion, that is, sudden short-term bursts of viral transmission caused by superspreader events, for instance, to be a more significant source of variation. On the other end of the spectrum is persistent heterogeneity, which refers to the individual behavioral characteristics pertaining to a long period of time, which is linked to a steadier fluctuation. They attempt to bring together both by considering both the biological and social nature of heterogeneity and their role in modifying epidemic dynamics throughout its time span, as well as how they determine the HIT and FSE.
The study says, “In our theory, a personal decision to attend a large party or a meeting would only be significant to the epidemic dynamics if it represents a recurring behavioral pattern. On the other hand, superspreading events are shaped by short-time variations in individual infectivity (e.g., a person during the highly infectious phase of the disease attending a large gathering).”
The latter would cause exaggerated estimates of heterogeneity compared to time-averaged or long-term measures that are important in determining how epidemics die out as herd immunity is attained.
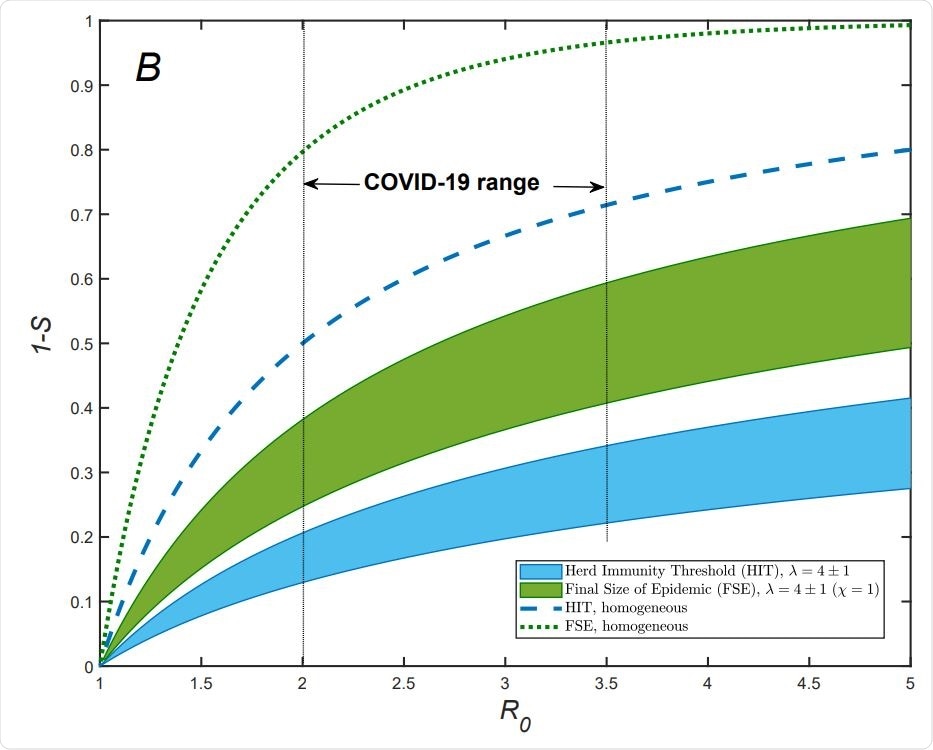
They comment that this approach is both “convenient and practically useful” in that it does not need more calibration to account for grossly changing epidemic conditions, but can incorporate real data. This is possible by incorporating the immunity factor λ, which encapsulates the whole effect of heterogeneity, in many cases. This factor decides how fast the effective reproduction rate, Re, falls in the early stage of the outbreak and is instrumental in arriving at the modified HIT and FSE in the absence of mitigation.
Sources of Heterogeneity
Heterogeneity among individuals in a population comes from biological factors, like immune function, genetic make-up, age and coexisting illnesses, and social factors, like the number of close social contacts one has. The susceptibility factor α would vary not only with biological immunity but would be higher in people in high-risk occupations such as healthcare workers, or in those who work in social hubs, or systematically defy social distancing regulations. These sources fall within the immunity factor λ.
Having estimated this, the researchers then used high-quality empirical data on hospitalizations, intensive care unit (ICU) occupancy, and the number of daily deaths to estimate the immunity factor λ, both from NYC and Chicago and from individual US states. They arrived at a marked decrease in Re, indicating the prominent role played by heterogeneity, and an immunity factor λ between 4 and 5. This closely agrees with the value calculated from social and biological heterogeneity. The researchers comment, “This analysis shows how our model is able to make concrete and testable predictions.”
Projections and Implications
The researchers incorporated their theory into a time-of-infection epidemiological model to predict the possible outcomes should a second wave occur in NYC and Chicago. Their projections are that there will be no second wave in NYC which means the HIT has already been passed there. In Chicago, which was hit with medium intensity, the second wave is projected to be much milder due to heterogeneity effects, even if no mitigation is undertaken. On the other hand, with mild measures such as wearing masks, limiting gatherings in indoor bars, dining areas, and other avenues for superspreader events, and tracing contacts, the second wave could be avoided altogether in such places, they suggest.
*Important Notice
medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
_facc0790943742e5b1cd51abaaaa0054-620x480.jpg)